The pediatric ot salary varies across sources, but most data show a clear range. A pediatric occupational therapist in the United States often earns between $63,000 and $104,000 per year, with the average pediatric occupational therapist salary commonly falling between $79,000 and $98,000, depending on job posting data and market trends.
According to the U.S. Bureau of Labor Statistics, the national average salary for occupational therapists is about $98,340, which provides a strong benchmark for pediatric OT roles within the broader field of occupational therapy. Pay typically ranges from $30 to $50 per hour, with higher rates seen in contract roles, per diem positions, or specialized settings. This pediatric ot salary range reflects full-time positions and may not include bonuses, benefits, or additional compensation such as health insurance. These numbers also change based on practice setting, location, experience, and other factors. A new grad entering the job market may start at a lower point, while experienced therapists or those working in higher-demand regions like Texas may earn more.
If you are actively exploring jobs, reviewing real openings, and comparing compensation can help you understand what you can expect. You can also review available roles through an occupational therapist staffing partner to see how current offers compare across settings.
Pediatric OT Salary Snapshot
The table below provides a clear overview of typical pediatric OT salary ranges based on experience and common job settings.
| Level | Annual Salary | Hourly Rate |
| Entry-level (new grad) | $63,000 – $75,000 | $30 – $36 |
| Mid-level | $75,000 – $95,000 | $36 – $45 |
| Experienced | $95,000 – $104,000+ | $45 – $50+ |
What a Pediatric Occupational Therapist Does
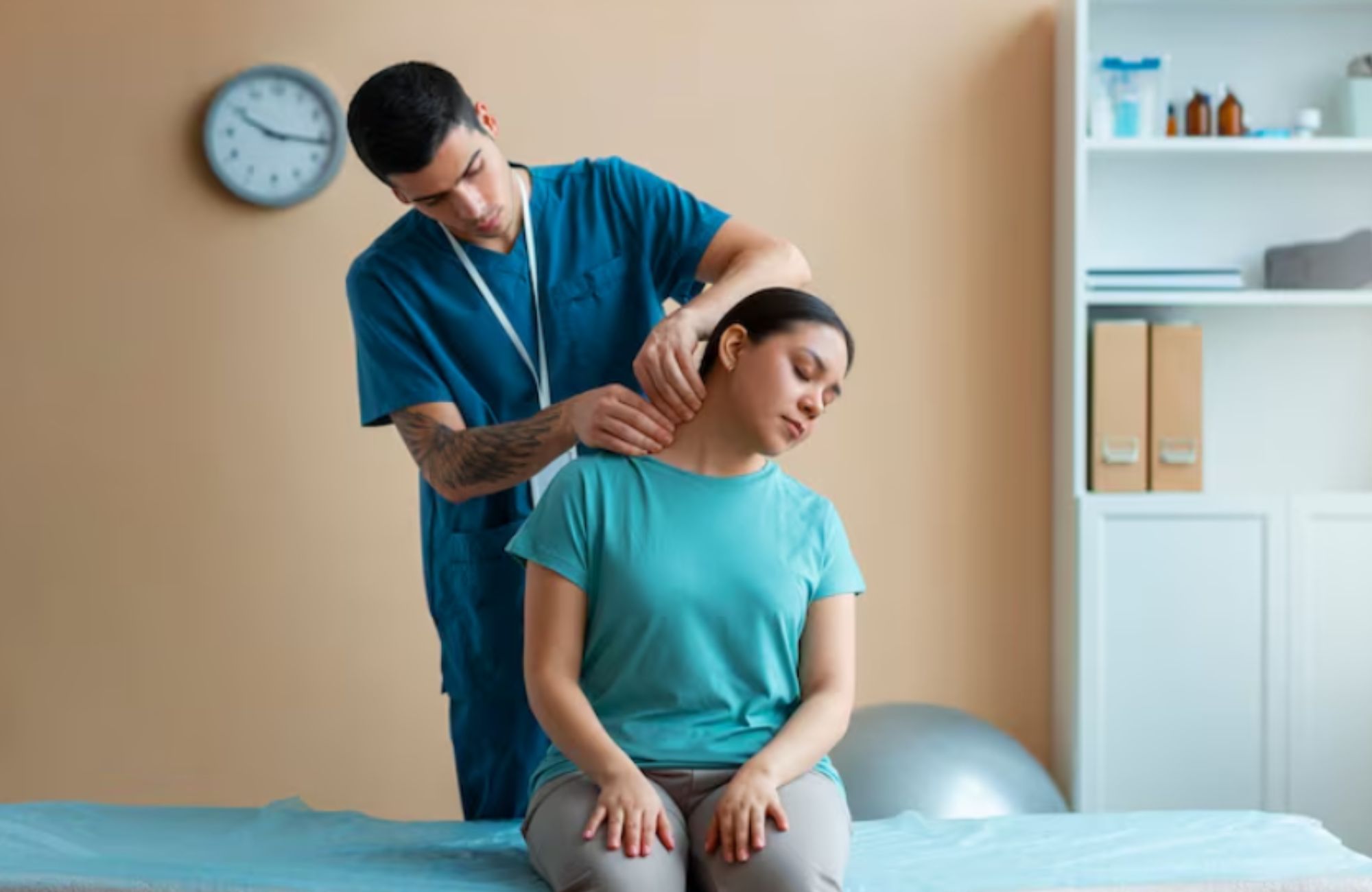
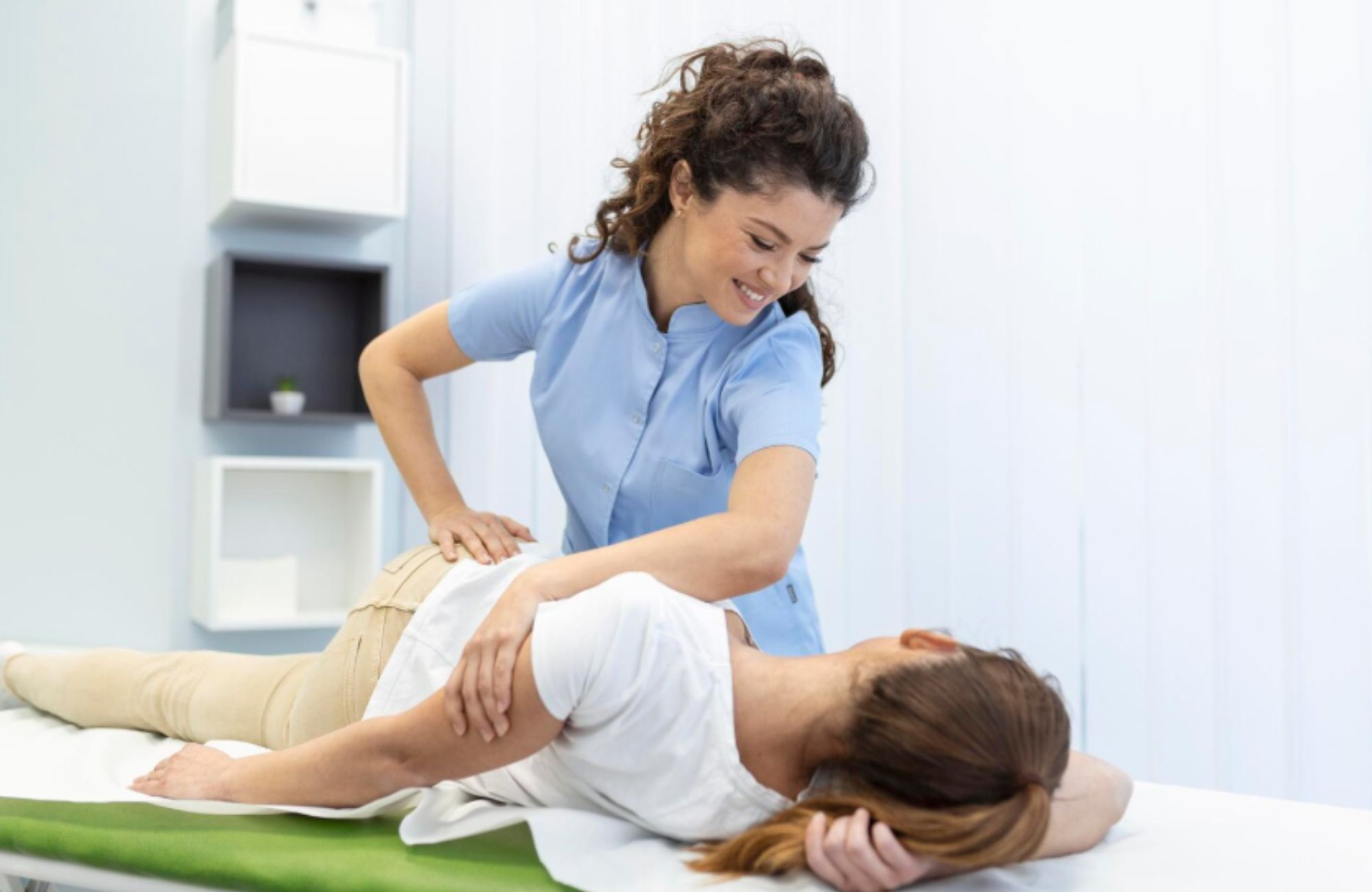
A pediatric occupational therapist works with children to improve daily function, independence, and participation in school and life. Pediatric OT focuses on helping kids build skills they need to complete everyday tasks, from holding a pencil to managing self-care. These therapists work closely with families, teachers, and healthcare teams to support development across physical, cognitive, and social areas.
The work is practical and goal-driven. Pediatric OT supports fine motor skills, coordination, sensory processing, and behavior regulation. Many therapists work in school, hospital, or clinic environments, while others provide care in homes or community programs. The setting often shapes the schedule, workload, and salary.
Common responsibilities include:
- Supporting fine motor and hand strength development
- Improving self-care tasks such as dressing and feeding
- Addressing sensory and behavioral challenges
- Helping students participate in classroom tasks
- Collaborating with teachers, parents, and other therapists
Why Pediatric OT Salary Varies So Much
The pediatric ot salary can vary widely because different data sources measure pay differently. Some salary pages use employer job postings, while others rely on survey data or broader occupational therapy averages. That is why one site may show a lower average salary, while another shows a higher number closer to $98,000.
Salary also depends on real-world factors. Pay is influenced by practice setting, experience, schedule, and employer type. Benefits such as health insurance, paid time off, and sick leave also affect total compensation. A higher hourly rate may not always mean higher overall earnings if benefits are limited.
Key factors that affect pediatric OT salary:
- Location and cost of living
- Practice settings such as a school, hospital, or clinic
- Years of experience and specialization
- Full-time vs work part-time schedule
- Contract or direct hire employment
- Employer demand and job market conditions
Pediatric OT Salary by Practice Setting
The practice setting plays a major role in determining pediatric ot salary. Different settings offer different pay structures, schedules, and benefits. Some offer stability and consistent hours, while others provide higher hourly pay but less security.
Understanding how settings compare helps therapists make better career decisions. A role with slightly lower base pay may offer stronger benefits, better work-life balance, or long-term growth. Others may offer higher pay through contract or diem work but require flexibility.
School-based pediatric OT jobs
School-based roles are common for pediatric OT. These jobs often follow a school calendar and provide stable hours. Pay may be lower than in some clinical settings, but benefits and predictable schedules are a strong advantage.
Hospital pediatric OT jobs
Hospital roles involve more complex cases and may include acute or specialty care. These positions may offer competitive salaries and structured benefits. Work can be more demanding and may require weekend or rotating schedules.
Outpatient pediatric therapy jobs
Clinic-based roles focus on regular therapy sessions and productivity targets. Pay can vary widely depending on the employer and caseload expectations. Larger companies may offer stronger benefits packages.
Early intervention and community roles
These roles often involve travel and home-based therapy. Pay may depend on reimbursement rates and scheduling flexibility. Therapists may manage their own schedules across the week.
Contract and per diem roles
Contract or diem roles often offer higher hourly pay, sometimes above the average. These positions can provide flexibility but may not include full benefits.
Practice Setting Comparison
| Setting | Pay Outlook | Benefits | Schedule |
| School | Moderate | Strong | Predictable |
| Hospital | High | Strong | Variable |
| Outpatient | Moderate to High | Varies | Structured |
| Early Intervention | Moderate | Varies | Flexible |
| Contract/Per Diem | High hourly | Limited | Flexible |
Pediatric OT Salary by Experience Level
Experience is one of the most consistent drivers of pediatric ot salary. A new grad may start with a lower offer while gaining confidence, while experienced therapists often command higher rates. Employers value efficiency, documentation accuracy, and the ability to manage caseloads independently.
Over time, therapists may move into advanced roles such as lead therapist or supervisor. These roles often come with increased pay and responsibility. Some may also specialize in areas such as feeding therapy or sensory integration.
Salary by experience:
| Experience Level | Salary Range |
| New grad | $63K – $75K |
| 3–5 years | $75K – $90K |
| 5–10 years | $90K – $104K |
| Leadership roles | $100K+ |
Pediatric OT Salary by Location
Location has a direct impact on pediatric ot salary. States with higher demand or higher cost of living often report higher pay. For example, states like Texas, Washington, and Maryland frequently appear in higher salary ranges. However, a higher salary does not always mean more usable income due to living expenses.
The job market also plays a role. Areas with fewer therapists may offer stronger pay to attract candidates. Urban areas may have more active jobs, while rural areas may offer incentives to fill positions.
Location impacts pediatric OT salary through several key factors, including cost of living, demand for pediatric OT services, insurance reimbursement rates, and the level of competition among employers hiring therapists.
How Education and Credentials Affect Salary
To become a pediatric occupational therapist, a master’s degree in occupational therapy is required. After completing their education and passing certification, therapists enter the workforce and begin gaining experience. Education is the entry point, but experience and setting often have a stronger impact on long-term earnings.
Additional training can support career growth. Specialized skills can help therapists qualify for higher-paying roles or advanced positions. However, not all certifications directly increase salary. It depends on the employer and setting.
What Employers Look for in Higher Paying Pediatric OT Jobs
Employers look for therapists who can manage caseloads, communicate clearly, and support children effectively. Strong candidates demonstrate practical experience and confidence in pediatric care. They also show the ability to collaborate with families and interdisciplinary teams.
Higher-paying roles often go to therapists who can handle complex cases and maintain consistent documentation. Employers also value reliability and flexibility.
Skills employers prioritize:
- Clinical reasoning and decision making
- Communication with families and teams
- Documentation accuracy
- Time management
- Collaboration with teachers and healthcare staff
How to Find Higher Paying Pediatric OT Jobs
Finding stronger opportunities requires a focused job search. Reviewing active jobs across different settings can help identify patterns in pay and benefits. Comparing offers is key, especially when evaluating total compensation.
Working with a specialized staffing agency can simplify the process. Agencies provide access to multiple openings, help match therapists with the right roles, and offer guidance during hiring.
Job search strategies:
- Compare multiple offers, not just one
- Evaluate total compensation, not just base salary
- Focus on settings that match your career goals
- Use staffing support to access more opportunities
If you are looking for a faster way to explore opportunities, reviewing open roles through a specialized staffing agency can provide insight into current market pay and available positions.
How to Negotiate Pediatric OT Salary
Negotiation is a key step in improving pediatric ot salary. Many therapists accept initial offers without asking questions, which can limit earning potential. Employers often expect negotiation, especially for experienced candidates.
Negotiation should focus on both salary and benefits. Clear communication and research-backed expectations can improve outcomes.
What to negotiate
- Base salary or hourly rate
- Benefits such as health insurance
- PTO and sick time
- Schedule flexibility
- CEU support
Common Pay Tradeoffs Pediatric OTs Should Understand
Higher pay often comes with tradeoffs. Some roles offer strong hourly rates but limited benefits. Others provide stability but lower pay. Understanding these tradeoffs helps therapists make better long-term decisions.
Debt and financial pressure can also influence choices. Many therapists graduate with loans, which can make higher-paying roles more appealing early in their careers.
Common tradeoffs in pediatric OT jobs include choosing between higher hourly pay with limited benefits, full-time stability versus flexible schedules, and balancing salary levels with workload demands and burnout risk.
Is Pediatric OT a Good Career for Earning Potential?
Pediatric OT offers stable career growth and consistent demand. Therapists work in a field that supports children and families, which adds meaning to the work. The profession also offers flexibility across settings.
At the same time, salary growth can feel slow in some roles. Many therapists report frustration with raises, especially early in their careers. Choosing the right setting and employer can improve long-term outcomes.
How Flagstar Rehab Helps Pediatric Occupational Therapists Find Better Opportunities
Flagstar Rehab supports therapists by connecting them with roles across multiple settings. This includes school-based, hospital, and clinic positions, as well as contract opportunities. Having access to multiple options helps therapists compare offers and find better fits.
The team also provides support throughout the hiring process. This includes matching candidates with employers, assisting with credentialing, and helping therapists prepare for interviews. Working with an ot staffing agency can improve visibility into the job market and reduce the time spent searching.
Conclusion
The pediatric ot salary range provides a starting point, but actual earnings depend on setting, experience, and job selection. Therapists who compare roles carefully and understand compensation factors tend to make stronger career decisions. Focusing on both salary and benefits leads to better long-term outcomes.
At Flagstar Rehab, we help pediatric occupational therapists find roles that align with their goals, whether you are a new grad or an experienced clinician. We provide access to opportunities across settings and support you through each step of the hiring process. Contact us to explore current openings and find the right fit for your career.
FAQs
What is the highest-paid OT job?
The highest-paid OT jobs are typically in home health, skilled nursing facilities, and specialized hospital roles. These settings often offer higher reimbursement rates and greater demand, which can increase overall pay. Leadership, management, and non-clinical positions can also offer higher salaries depending on experience and responsibility.
What type of OTs get paid the most?
OTs working in contract, travel, or per diem roles often earn higher pay due to flexibility and demand. Therapists in high-paying settings or underserved areas may also receive stronger compensation packages. Experience, specialization, and location all play a major role in how much therapists earn.
Is OTA a low-stress job?
OTA roles can vary in stress depending on the setting, caseload, and employer expectations. Some positions offer stable schedules and supportive environments, while others may involve higher productivity demands. Job satisfaction often depends on workload, team support, and work-life balance.
Where do pediatric occupational therapists make the most money?
Pediatric occupational therapists tend to earn more in states with higher demand, such as Texas and California. Hospital settings and contract roles may also offer higher pay compared to school-based positions. Working with a staffing partner can help identify higher-paying opportunities across different locations and settings.